What is PRP?
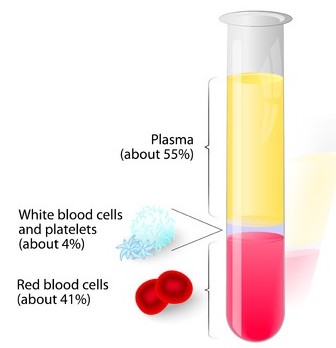
PRP is an autologous concentration of human platelets to supraphysiologic levels. Platelets are irregularly shaped, nonnucleated cytoplasmic bodies derived from fragmentation of megakaryocyte precursors. PRP is a specialized form of blood plasma that is rich in growth factors, cytokines, and stem cell precursors.
The growth factors from PRP promote cell differentiation and maturation. When combined with a stem cell treatment, the stem cells are like planting the seeds and the PRP is like the soil, water, fertilizer, and sunlight that help the seeds mature and grow.
As part of our patented TBI Therapy Protocol, insulin and PRP infusions can be administered in coordination with another regenerative injection therapy – stem cell therapy – to help accelerate regrowth and rehabilitation in the brain.
Benefits of PRP
- Regrowth of brain collagen (proteins that provide strength and structure)*
- Activation and targeting of stem cells (cellular regeneration and differentiation)*
- Increased angiogenesis (the development of new blood vessels)*
- Decreased inflammation (increasing brain functionality)*
- Reduction of amyloid proteins (which result in memory loss)*
*Results may vary; no guarantee of specific results

At baseline levels, platelets function as a natural reservoir for growth factors, including platelet-derived growth factor (PDGF), epidermal growth factor (EGF), transforming growth factorbeta 1 (TGFβ1), vascular endothelial growth factor (VEGF), basic fibroblast growth factor (FGF), hepatocyte growth factor (HGF), and insulin-like growth factor (IGFI). There is a general consensus in PRP research that the injection of concentrated platelets, once activated, results in an exponential increase in numerous growth factors at the sight of PRP injection.
Intranasal PRP Procedure
Patients present for a 3-day program are recommended to receive at least 2 HBOT dives before doing IN PRP. If possible, with time and patient permitting, it is recommended that patients get a second IN PRP/insulin/glutathione/B12 (PRP cocktail) treatment (or IN stem cell treatment) after the first treatment. For moderate to severe TBI patients, it is recommended to get an IN PRP cocktail every 2-3 weeks while completing a 40 HBOT series. If patients are local and unable to afford such treatment, getting a IN PRP every 1-2 months, in combination with home HBOT, for a total of 3-4 treatments in 6 months is acceptable.
PRP is harvested from the patient’s blood by a simple blood draw. During infusion, the patient will lay back on the exam table with their head tilted perpendicular to the ground. After local anesthetic is sprayed into the nose, the PRP combined with insulin and other nutrients is dripped up the nose with a special device. The patient will lie there for another 15 minutes while the PRP fuses into the brain. After this, the patient is free to get up and continue their daily activities.
To promote optimal regeneration, PRP is usually paired with several hyperbaric oxygen therapy (HBOT) sessions before and after. The PRP is infused the day before the intranasal stem cell infusion.
How Do Growth Factors in PRP Aid Healing?
PDGF (Platelet-Derived Growth Factor):
- Macrophage activation and angiogenesis
- Fibroblast chemotaxis and proliferative activity
- Enhances collagen synthesis
- Enhances the proliferation of bone cells
IGF1 (Insulin-Like Growth Factor-I):
- Chemotactic for myoblast and fibroblasts and stimulates protein synthesis
- Mediator in growth ad repair of skeletal muscle
- Enhances bone formation by proliferation and differentiation of osteoblasts
TGFp (Transforming Growth Factorβ):
- Enhances the proliferative activity of fibroblasts
- Stimulates biosynthesis of type I collagen and fibronectin
- Induces deposition of bone matrix
- Inhibits osteoclast formation and bone resorption
- Regulation in balance between fibrosis and myocyte regeneration
PDEGF (Platelet-Derived Endothelial Growth Factor):
- Promotes wound healing by stimulating the proliferation of keratinocytes and dermal fibroblasts
PDAF (Platelet-Derived Angiogenic Factor)
- Induces vascularization by stimulating vascular endothelial cells
EGF (Endothelial Growth Factor):
- Cellular proliferation
- Differentiation of epithelial cells
VEGF (Vascular Endothelial Growth Factor)
- Angiogenesis
- Migration and mitosis of endothelial cells
- Creation of blood vessel lumen
- Creation of fenestrations
- Chemotactic for macrophages and granulocytes
- Vasodilation (indirectly by release of nitrous oxide)
HGF (Hepatocyte Growth Factor):
- Stimulates of hepatocyte proliferation and liver tissue regeneration
- Angiogenesis
- Mitogen for endothelial cells
- Antifibrotic
Safety and Side Effects
Bloody noses and swallowing plasma or local anesthesia have been the biggest side-effects of IN PRP. If the patient swallows the PRP/insulin/nutrient cocktail, he or she may need some form of sweet substance to eat to prevent a drop in blood sugar. Sneezing is another danger of the treatment. Using good sterile technique will prevent infection.
